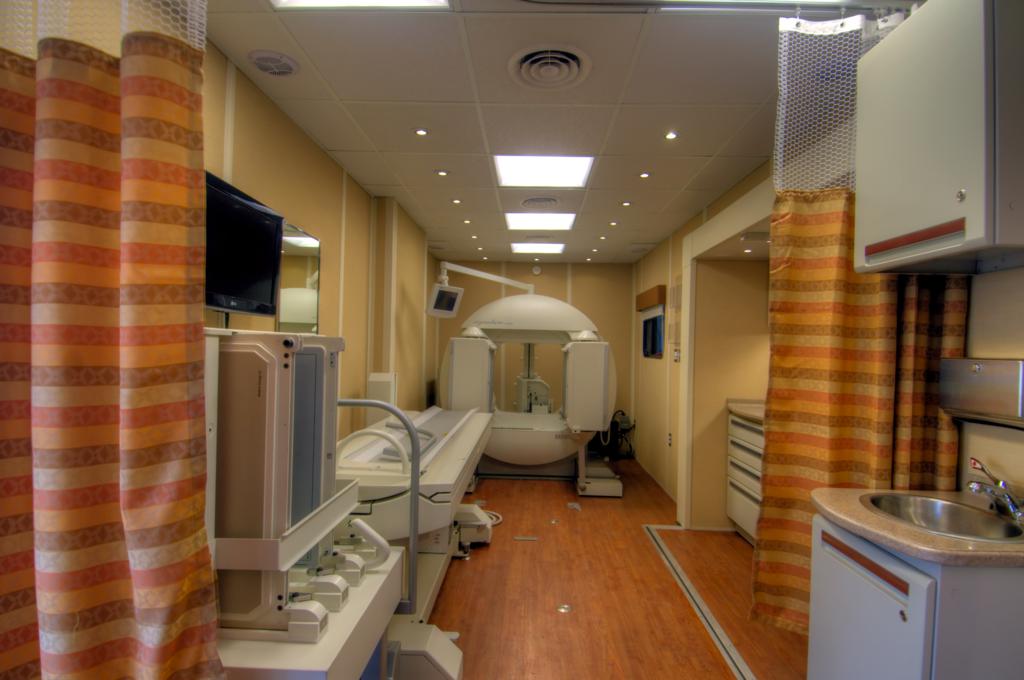
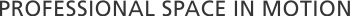Custommade medical clinics use onboard technologiesthat combine to allow medical access to a broader population. According to the World Health Organization the demand for these vehicles is continuously rising due to their numerous benefits and their ability to fulfill the needs of an increasing population. Studies have reported a recent shortfall of 90,000 physicians and untold number of nurses in the U.S.,while there is ananticipated increase in new patients of 28 million by 2050. Taking this into account, clinical workflows must improve, and medical institutions and providers must adapt to his changing environment.
Combination Mobile Medical and Dental Clinics Provide Dual Care
Topics: mobile dental, Mobile Medical, Combination Mobile Medical and Dental Clinics
Mobile Diabetes Clinics: Case Studies & Justifications
Mobile medical serves the entire range of at risk populations around the world; from disenfranchised African-Americans with diabetes - to the homeless - to children living in rural environments who lack health insurance - to indigenous communities - to isolated and impoverished people in the Middle East. Sometimes MHCs are the provider of last resort when mainstream healthcare fails to engender trust in a community or in areas where there are not any accessible health provider services.
Topics: Mobile Medical, Mobile Health Clinic, Mobile Diabetes Clinics
3 Healthcare Institutions that Benefit from Mobile Medical
The model of mobile medical is to provide cost-effective, high quality care, many times to disenfranchised populations in underserved areas.
Topics: Mobile Medical Clinics, Mobile Medical, Continuity of Care with Mobile Health Clinics, Mobile Health Clinic
2 Ways to Preserve & Grow Your Market Share with Mobile Clinics
If you only have 5 percent of the healthcare market in your service area, imagine if you edged up just 1 point to 6 percent. That is 20 percent growth for your FQHC or hospital. Consider a mid-sized hospital system with $350 million in revenues, that 20 percent growth is a significant $70 million.
Topics: mobile mammography, Mobile dentistry, Mobile Medical, Continuity of Care with Mobile Health Clinics
Building Continuity of Care with Mobile Health Clinics
A mobile health clinic provides innovative and flexible healthcare delivery to vulnerable, rural, urban and generally underserved populations. Though often misunderstood, and sometimes not fully utilized, mobile health units can provide continuity of care in a number of ways, including:
Topics: mobile mammography, Mobile dentistry, Mobile Medical, Continuity of Care with Mobile Health Clinics
Mobile medical clinics are customized vehicles which typically travel to urban and rural communities, many times targeting underserved low-income and minority populations who have a disproportionate burden of ill health and would benefit the most from the care provided to them by a mobile clinic. Other mobile units offer pediatric services at schools for immunizations, asthma screening, vision screening, and more. Most times, the goal is to deliver primary care for people who don’t have a healthcare home, or who cannot or will not seek preventive care. In the school setting, healthcare professionals can spot problems that parents don’t see. Mobile clinics are an integral component of the broader healthcare systems throughout the world, serving vulnerable populations and promoting high-quality care at low cost in the Americas, Europe, Africa, the Middle East, Ukraine and beyond.
Topics: Mobile Medical Clinics, Mobile Medical