Traditionally we think of Mobile Health Clinics (MHCs) being utilized to provide healthcare services to underserved populations. We know that MHCs improve outcomes and reduce costs related to healthcare delivery and provide access to care by delivering services to populations that are historically underserved. Yet how often do we consider the impact MHCs can have on emergency preparedness and disaster relief in times of crisis? Working to help form the United Nations after WWII Winston Churchill famously said, “Never let a good crisis go to waste”. This was not a cynical comment. He was making the clear point that in the wake of World War II allied countries should come together to form an alliance to stave off the potential of future disasters. To be prepared.
Disaster Relief & Emergency Preparedness: Role of Mobile Health Clinics
8 Critical Mistakes People Make in Mobile Medical Start-Ups
Urgent care clinics have seen a record number of patients since 2020, and the high volumes don’t seem to be going anywhere. This coupled with changes in the population and their healthcare needs, a growing shortage of physicians and other healthcare professionals, and hospitals closing in rural areas all demonstrate an increasing demand for mobile health clinics. The awareness of these changes has driven many healthcare organizations to pursue mobile clinics as a major part of their services portfolio.
Topics: mobile mammography, mobile dental, Mobile Health Clinic, Planning a successful mobile medical clinic
The Cancer Moonshot Initiative and Out-of-Office Cancer Screenings
Mobile health care serves a wide section of the population providing dental care, blood donations, primary and preventive medical care, along with mobile mammography and general cancer screenings. We all know cancer screenings are important for the early detection of disease, better health outcomes, and saving more lives. Many organizations work with the CDC through their national programs to extend these services to millions of people.
Topics: mobile breast cancer screening unit, mobile mammography, Mobile Health Clinic, Cancer Screenings
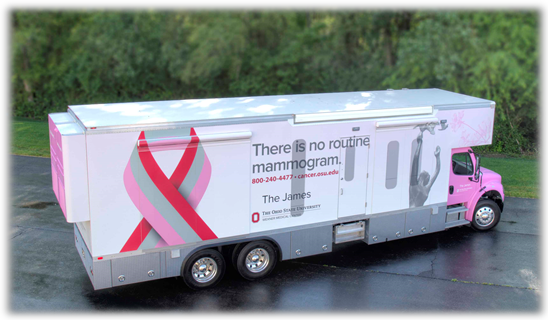
Mobile Health Clinics Provide Care in the United States
With more than 2,000 on the road in the U.S. and performing 6-½ million visits annually mobile health clinics serve an important role in the health care system, providing care to some of the most vulnerable populations. Between 2007 and 2017 Mobile Health Map monitored 811 participating clinics to identify:
Topics: Mobile Medical Clinics, Mobile Health Clinic, Mobile Health Clinics in the U.S.
Mobile Medical: On the Frontlines of Healthcare Delivery
For decades mobile clinics are a relatively untapped resource for global healthcare. In 2020 and beyond, the COVID-19 pandemic exhibits the important role of mobile health clinic programs. They provide critical access to healthcare professionals, especially for disenfranchised communities. They serve to fill the gap as a safety-net in what is often a deficient healthcare infrastructure, reaching social and economically underserved populations in urban and rural areas.
Topics: Mobile Medical Clinics, Mobile Health Clinic, Mobile clinic COVID-19 safety
Mobile Medical: Quick Ways to Boost Income and Power Your Bottom Line
Topics: Mobile Health Clinic, Mobile Medical Clinic, Mobile Clinic Marketing
Mobile Health Clinics Can Play a Major Role in Smoking Cessation
According to the Centers for Disease Control and Prevention more than 16 million Americans are living with a disease caused by smoking. It is common knowledge that smoking causes cancer, heart disease, stroke and lung diseases. The FDA states that almost 70 percent of current smokers report wanting to quit smoking, however fewer than half makes it past an attempt. Receiving guidance from a healthcare provider to quit is often the only way many people will make the attempt and follow through.
Topics: Mobile Health Clinic, Smoking Cessation
Mobile Diabetes Clinics: Case Studies & Justifications
Mobile medical serves the entire range of at risk populations around the world; from disenfranchised African-Americans with diabetes - to the homeless - to children living in rural environments who lack health insurance - to indigenous communities - to isolated and impoverished people in the Middle East. Sometimes MHCs are the provider of last resort when mainstream healthcare fails to engender trust in a community or in areas where there are not any accessible health provider services.
Topics: Mobile Medical, Mobile Health Clinic, Mobile Diabetes Clinics
Mobile Medical Reduces Unnecessary Emergency Room Visits
Topics: Mobile Health Clinic, Mobile Medical Clinic, Unnecessary Emergency Room Visits
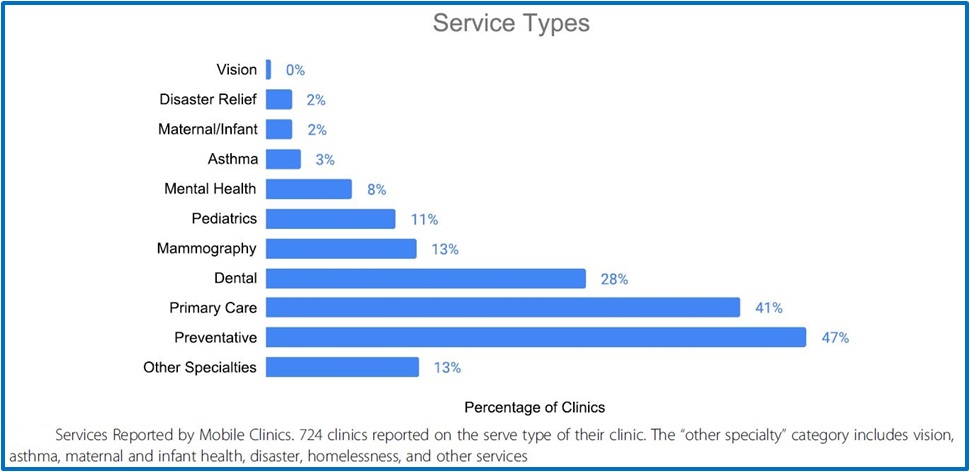
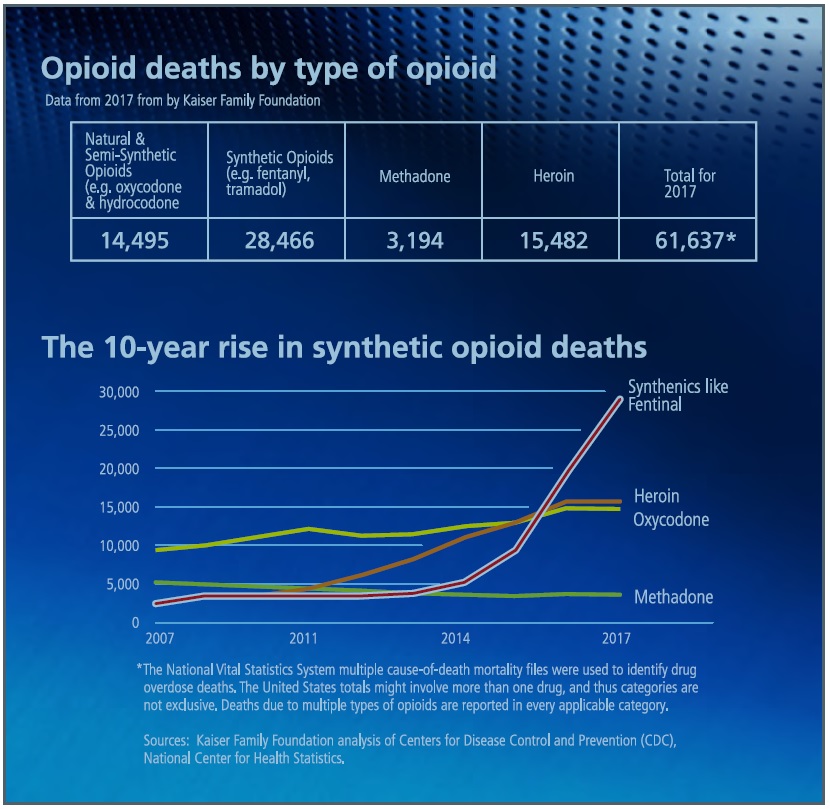
HRSA Grants Fund Mobile Health Clinics for Fighting Opioid Addiction
In 2017, drug overdose deaths in the United States were more than 70,000, which is almost 200 per day. This was nearly a 10 percent increase from 2016.
Topics: Mobile Medical Clinics, Mobile Health Clinics for Behavioral Health, Mobile Health Clinic, Mobile Health Clinics Fight Opioid Addiction