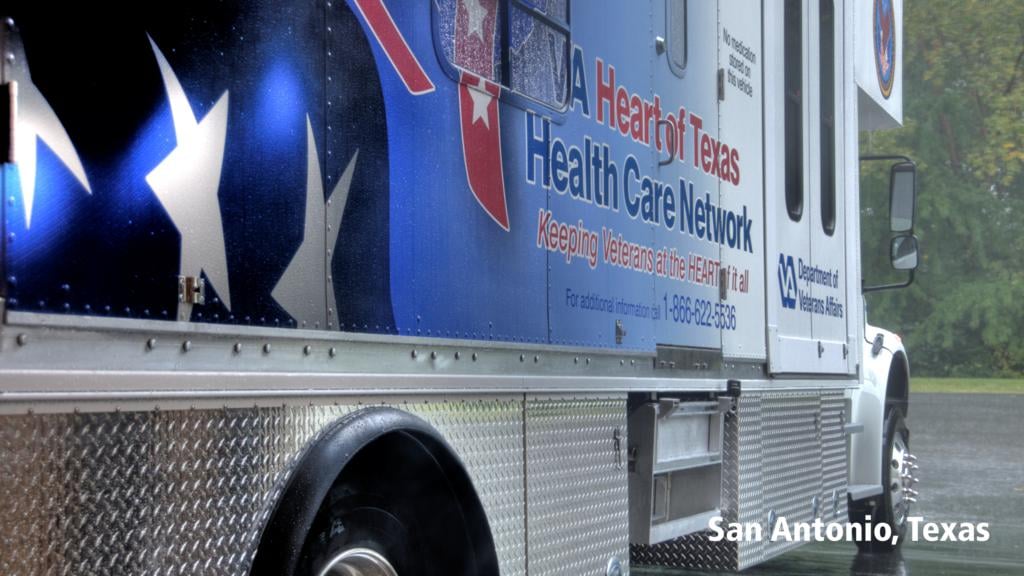
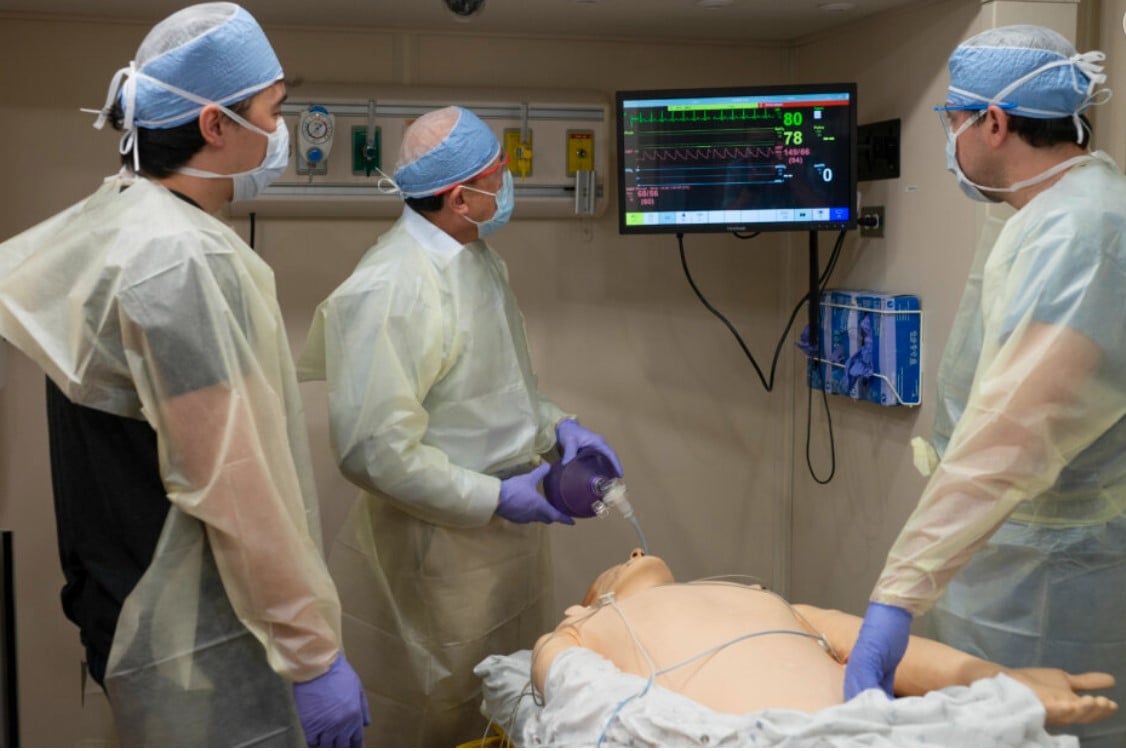
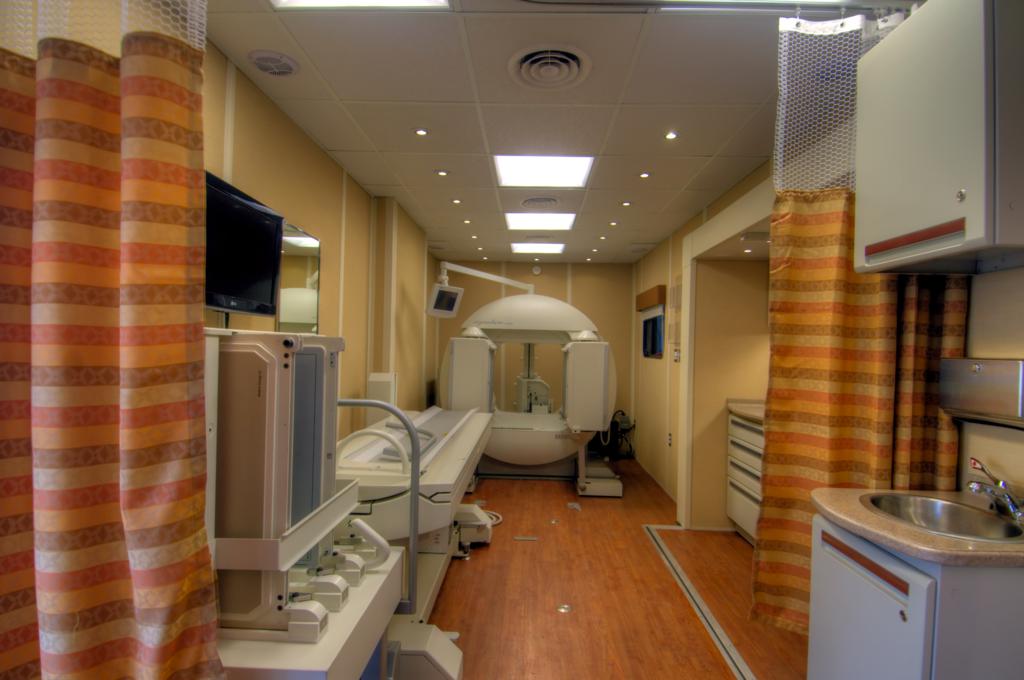
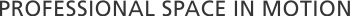For the past twenty-five years, there has been a significant increase in the use of simulation-based training for healthcare providers. Today, simulation technology advancements have become a primary component of medical education. With the increasing complexities in healthcare, simulation-based training (SBT) enhances clinical skills and patient safety.
Lee Guse
Recent Posts
8 Reasons to Use Mobile Units for Simulation Training
Topics: Mobile Sim Labs, Healthcare Simulation
Access to Medical and Behavioral Care For Children: A National Crisis
A primary goal of the U.S. health system is to provide affordable, value based, accessible care. Healthcare services are largely provided by hospitals and clinics, yet, among all of the methods for healthcare delivery mobile health clinics are the most effective in providing care to underserved children, offering a unique solution to expanding health equity and improving quality of care. There is a growing emphasis by the healthcare community to provide more stable medical services to children, particularly post pandemic.
Topics: Mobile Medical Clinic, Mobile Medical for Behavioral Health Programs, Mobile Medical Clinics for Behavioral Health
Mobile Behavioral Health & Addiction Clinics: Battling the Stigma
“Mental illness is nothing to be ashamed of, but stigma and bias shame us all.”
Over forty years ago, Sister Bernadette Kenny of the Catholic Order Medical Missionaries would drive her Volkswagen Beetle through the rural mountain roads of Appalachia to deliver health care to remote and disenfranchised people. Sister Kenny’s efforts eventually became a $3.6 million organization known as Central Appalachia’s Saint Mary’s Health Wagon, providing a number of healthcare services, including mobile behavioral health clinics.
Topics: Mobile Medical Clinic, Mobile Medical for Behavioral Health Programs, Mobile Medical Clinics for Behavioral Health
Disaster Relief & Emergency Preparedness: Role of Mobile Health Clinics
Traditionally we think of Mobile Health Clinics (MHCs) being utilized to provide healthcare services to underserved populations. We know that MHCs improve outcomes and reduce costs related to healthcare delivery and provide access to care by delivering services to populations that are historically underserved. Yet how often do we consider the impact MHCs can have on emergency preparedness and disaster relief in times of crisis? Working to help form the United Nations after WWII Winston Churchill famously said, “Never let a good crisis go to waste”. This was not a cynical comment. He was making the clear point that in the wake of World War II allied countries should come together to form an alliance to stave off the potential of future disasters. To be prepared.
Mobile simulation labs have the latest medical equipment used in emergencies, trauma situations and everyday patient care. These training centers on wheels simulate ambulance, emergency room and hospital patient care settings. They use computerized high-fidelity patient simulator manikins that can breathe, respond to treatment, and even talk. The medical trainees use actual medical and rescue equipment, including cardiac monitors and defibrillators, resuscitation equipment, airway management equipment, intravenous supplies and more. Mobile sim labs provide personnel with the experience of a wide variety of standardized scenarios and practices for multiple procedures, delivering the highest quality of experiential learning for those on the frontlines.
Topics: Mobile Sim Labs, Simulation Lab, Healthcare Simulation, Mobile Simulation Funding
Mobile Health Care Act: Federal Funds for Mobile Healthcare
On October 18, 2022, the MOBILE Health Care Act was signed into law. This bipartisan, bicameral legislation Maximizing Outcomes through Better Investments in Lifesaving Equipment for MOBILE Health Care Act will broaden the ability to provide much needed healthcare services to rural and urban communities. The legislation, which takes effect on January 1, 2024, will allow health centers to use federal funds in establishing mobile healthcarefor their communities to increase access to medical services for underserved populations.
Topics: Mobile Medical Clinics, Mobile Health Clinics, Mobile Health Care Act
Mobile Clinics Provide Vital Cancer and Cardiovascular Screenings
Regardless of the pandemic there has always been an urgent need for adaptable healthcare interventions for the underserved. Interventions that improve health outcomes and address the inequality for those on the fringes of society. The topic of health equity always comes around to: “Meet people where they are”. This refers to bringing accessible healthcare to people where they live and work, and most particularly to the urban and rural poor. However, regardless of this general consensus, much of the medical community has yet to embrace the most useful instrumentality of meeting people where they are with Mobile Medical Clinics.
Topics: Mobile Medical Clinic, Cancer Screenings, Cardiovascular Screenings, Nuclear Medicine
Funding Opportunities for Mobile Medical Simulation Training
The learning and development requirements in healthcare are considerably different than other businesses. Training to care for the human body is challenging for talent development in healthcare. And trainees are extremely segmented with differing needs, ranging from:
Topics: Simulation Lab, Healthcare Simulation, Mobile Simulation Funding
Mobile Medical Clinic Funding for Behavioral Health Programs
The burden of mental, behavioral, and substance use disorders on disenfranchised people has exceeded the capacity of today’s healthcare systems, particularly in the wake of the COVID-19 pandemic. As many as 75 percent of people with serious mental illness in low income regions, such as rural and urban settings, cannot easily access basic treatment services. However, mobile clinics have successfully proven their usefulness in providing treatment for depression and other behavioral health issues, substance abuse, traumatic stress disorder, and even alcohol-use disorders. According to the National Library of Medicine, Mobile medical clinics represent an untapped resource for our healthcare system.
Topics: Mobile Health Clinics for Behavioral Health, Funding Mobile Medical for Behavioral Health
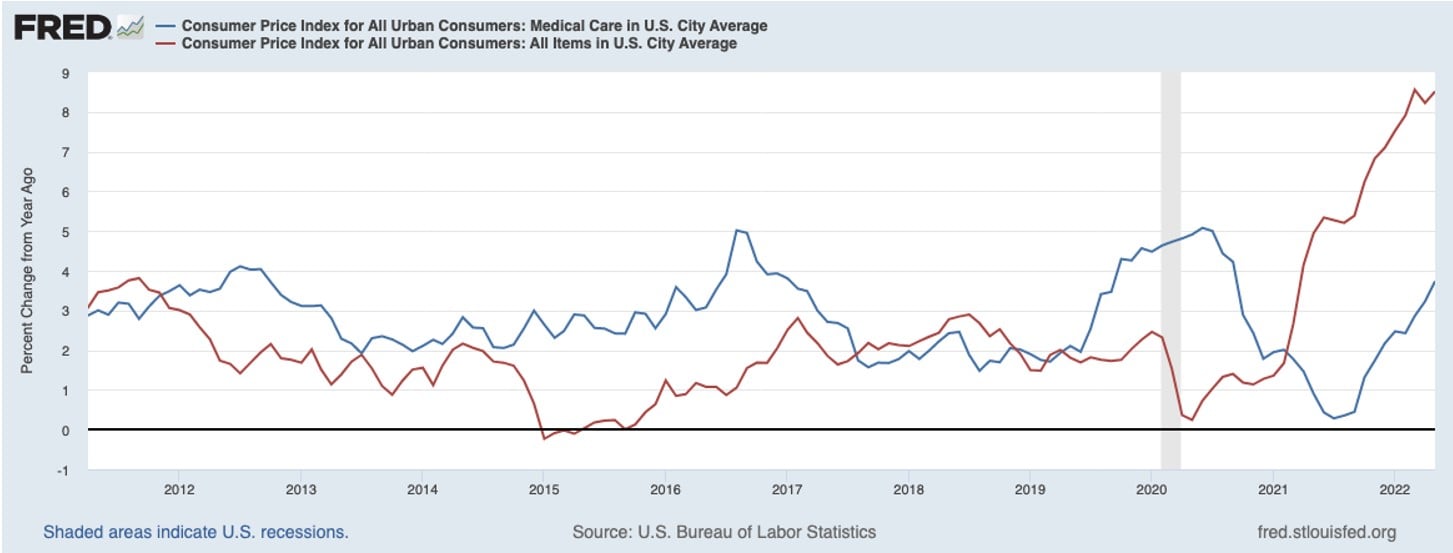
How Can Mobile Medical Clinics Help During Inflationary Times?
With faltering economic recovery, many industries are scrambling to deal with continued supply shortages, increasing commodity prices, and higher wages triggered by labor shortages. In 2021 the producer price index (PPI) rose 10% in the industrialized world. The PPI measures the postproduction prices of goods and is a barometer of the pressures on manufacturing. The last time there was this level of increase in PPI was in the first half of 2008.
Topics: Mobile Medical Clinics, Inflation