Recently the U.S. Department of Health and Human Services (HHS) announced a landmark Maternal Health Initiative. The initiative incorporates a comprehensive HHS Action Plan to significantly reduce maternal deaths and disparities that put women at risk before, during and after pregnancy. In addition the U.S. Surgeon General issued a corresponding Call to Action to Improve Maternal Health, which puts forth the critical roles healthcare providers can do to improve maternal health, which should include mobile medical.
Call to Action for Maternal Health: Mobile Clinics Provides Solution
Topics: Call to Action to Improve Maternal Health, Maternal Mortality and Morbidity
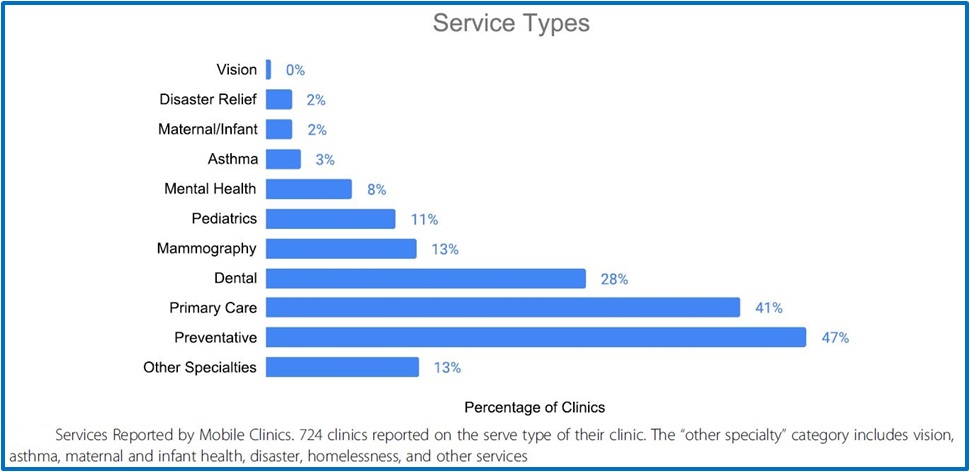
Mobile Health Clinics Provide Care in the United States
With more than 2,000 on the road in the U.S. and performing 6-½ million visits annually mobile health clinics serve an important role in the health care system, providing care to some of the most vulnerable populations. Between 2007 and 2017 Mobile Health Map monitored 811 participating clinics to identify:
Topics: Mobile Medical Clinics, Mobile Health Clinic, Mobile Health Clinics in the U.S.
Mobile Medical: On the Frontlines of Healthcare Delivery
For decades mobile clinics are a relatively untapped resource for global healthcare. In 2020 and beyond, the COVID-19 pandemic exhibits the important role of mobile health clinic programs. They provide critical access to healthcare professionals, especially for disenfranchised communities. They serve to fill the gap as a safety-net in what is often a deficient healthcare infrastructure, reaching social and economically underserved populations in urban and rural areas.
Topics: Mobile Medical Clinics, Mobile Health Clinic, Mobile clinic COVID-19 safety
It’s important for the health and safety of your community to keep your mobile health clinic operating during the COVID-19 health crisis. However, the confines of a mobile clinic can be perceived as a fearful environment for some health care providers and patients. To address these concerns advancements have been made in developing several methods to protect medical staff and the public while inside a mobile clinic.
Topics: Mobile clinic COVID-19 safety
Mobile Health Clinics around the world are being used for COVID-19 testing, from Poland and Latvia to Argentina and the U.K. Plus, all over the United States mobile clinics have been built specifically for testing. Or in many cases clinics normally used for dentistry or childhood immunizations have reconfigured and/or directly redeployed to test individuals for the novel coronavirus.
Mobile Medical: Quick Ways to Boost Income and Power Your Bottom Line
Topics: Mobile Health Clinic, Mobile Medical Clinic, Mobile Clinic Marketing
Mobile Health Clinics Can Play a Major Role in Smoking Cessation
According to the Centers for Disease Control and Prevention more than 16 million Americans are living with a disease caused by smoking. It is common knowledge that smoking causes cancer, heart disease, stroke and lung diseases. The FDA states that almost 70 percent of current smokers report wanting to quit smoking, however fewer than half makes it past an attempt. Receiving guidance from a healthcare provider to quit is often the only way many people will make the attempt and follow through.
Topics: Mobile Health Clinic, Smoking Cessation
Mobile Diabetes Clinics: Case Studies & Justifications
Mobile medical serves the entire range of at risk populations around the world; from disenfranchised African-Americans with diabetes - to the homeless - to children living in rural environments who lack health insurance - to indigenous communities - to isolated and impoverished people in the Middle East. Sometimes MHCs are the provider of last resort when mainstream healthcare fails to engender trust in a community or in areas where there are not any accessible health provider services.
Topics: Mobile Medical, Mobile Health Clinic, Mobile Diabetes Clinics
Mobile Medical Reduces Unnecessary Emergency Room Visits
Topics: Mobile Health Clinic, Mobile Medical Clinic, Unnecessary Emergency Room Visits
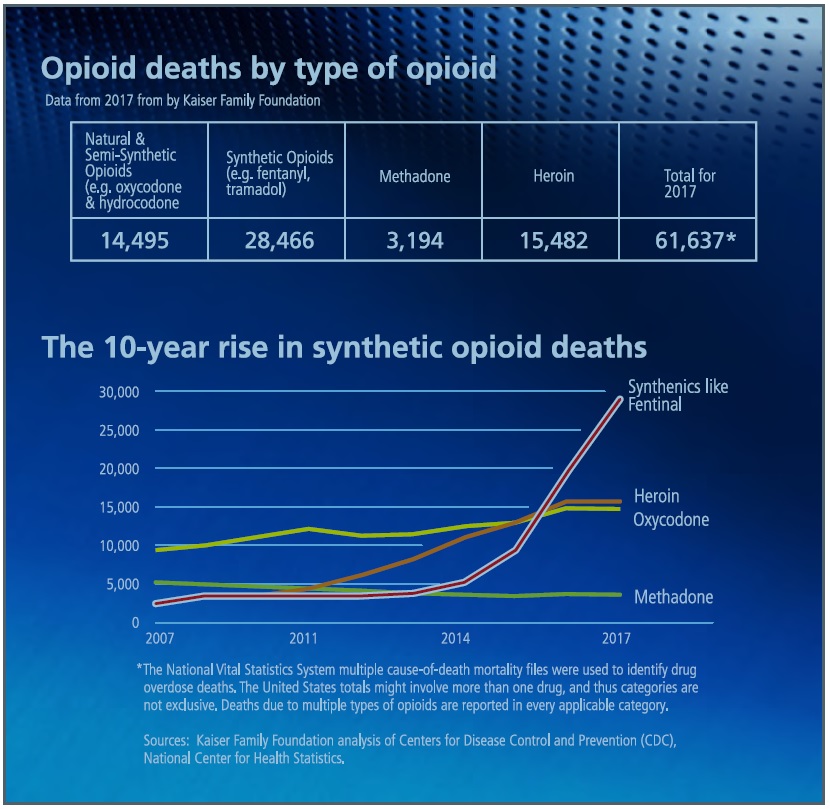
HRSA Grants Fund Mobile Health Clinics for Fighting Opioid Addiction
In 2017, drug overdose deaths in the United States were more than 70,000, which is almost 200 per day. This was nearly a 10 percent increase from 2016.
Topics: Mobile Medical Clinics, Mobile Health Clinics for Behavioral Health, Mobile Health Clinic, Mobile Health Clinics Fight Opioid Addiction